
The ONLY Probiotics to Take with Antibiotics
By a guest author
First, a note from Kelly: Remember, neither the author nor I are health professionals! Use what you read here for your own research and find what is best and right for YOU. Read my entire disclaimer here…
Knowing how they can harm our immune system, as much as we'd like to avoid it, there are times we still might need an antibiotic. Today find out the truth about which probiotics to take with antibiotics, BUT you've probably been told never to do that because it cancels out the effects…
Turns out, it's NOT ALWAYS TRUE! There are two probiotics to take with antibiotics that not only CAN be taken at the same time, but they really should be:
- Gut commensal spore bacteria — go here to get the probiotic that Kelly and I take and
- Saccharomyces Boulardii, a probiotic fungi.
The advantages to these antibiotic-resistant, yet health-supporting, microorganisms go far beyond the convenience of being able to take your pills at the same time (antibiotic + probiotic), rather than hours apart…
1. Probiotics to Take with Antibiotics: Gut Commensal Spore Bacteria
This category of bacterial strains is not new to the medical world, just new to the U.S. (Read more here: Is My Probiotic Really Helping or am I Wasting Money?)
Physicians in Europe and Asia have routinely written prescriptions since the 60's for this kind of spore bacteria probiotic to soothe the digestive irritation caused by the antibacterial medication. Both the pharmaceutical and the probiotic are taken at the same time with no negative effect on the probiotic or decrease in benefit to the patient.
Then why haven't we seen this more convenient kind of spore probiotic in this country before?
These strains are difficult and expensive to manufacture and so, despite decades of safe and effective use abroad, manufacturers over here for the most part opted to go with the easier and cheaper vegetative strains.
What's a “vegetative” strain?
A vegetative strain is bacteria that lacks any kind of protective spore shell. Currently about 99+% of conventional retail probiotics consist entirely of vegetative strains like the ones you've probably heard of: Lacto, Bifido, Streptococcus, etc.
Conventional probiotic strains…
- Have NO natural, protective shell, and so are delicate and easily killed by medications (including antibiotics), heat, stomach acid, etc. This fragility is why many of these probiotics must be kept in the frig and taken separately from antibiotics. They also…
- Cannot colonize in the oxygen-free environment of the gut. In terms of reproduction, it doesn't matter if vegetative bacteria survive stomach acid or not because all are produced in an environment that contains oxygen (including either a lab or through the fermenting of food). As a result, vegetative strains become genetically altered into aerobic (oxygen-based) versions that CANNOT bind to necessary receptor sites in the intestines and so, cannot colonize the anaerobic (oxygen-free) intestines.
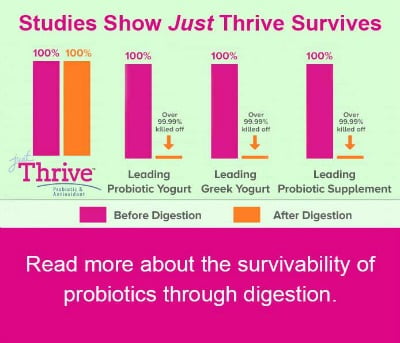
However, during and after antibiotics, hardy gut commensal spore bacteria survive and can guard our microbiome to prevent regrowth of the “bad guys.”
As we know, taking antibiotic medication is comparable to using a flame thrower on our microbiome garden. And luckily, while antibiotics can never kill ALL the bacteria in our gut (think how large and convoluted are your intestines with so many folds and corners), it does leave the population very, very low – good and bad bacteria equally destroyed.
Once we finish a round of antibiotics we are at HUGE RISK for actually becoming sicker than we were before we began the medication.
Post-antibiotic, the beneficial strains in our gut have been so eradicated they can no longer prevent the wildfire regrowth of pathological microbes. So what often takes over like a weed?
- Harmful bacteria, especially the particularly hardy “superbugs,” and
- Candida and other harmful fungi unaffected by antibiotics.
But because the gut commensal spore bacteria survive, they:
- Stand guard over the few remaining beneficial strains, feeding them nutrients to strengthen them, and
- Kill any harmful bacteria that attempt to regrow.
 How do I know if my probiotic is not Vegetative or Soil-Based strains?
How do I know if my probiotic is not Vegetative or Soil-Based strains?
***Go here to get the probiotic that Kelly and I take.*** Use the code KOP for a discount — if you order 3 or more, it's an even better deal than their auto-ship option + you'll get free shipping!
It's designed to take before, during, and after antibiotics, or as ongoing gut protection. All four strains in here are 100% gut commensal spore bacteria.
What kind of probiotic do you have? Just look on the ingredient label:
- A spore (naturally having a shell) bacteria will always start with “Bacillus” followed by the latin name of the strain.
- If the name starts with anything else, it is either a vegetative (no shell, very fragile) bacteria or possibly a probiotic fungi (more on this later).
*Spore bacteria can be either soil-based OR gut commensal:
- Soil-based organisms (S.B.O.) consists of bacteria, either vegetative or spore, whose natural home is the earth. Dirt is where they find food and reproduce, the end result being increased soil fertility. Similar to vegetative strains, however, soil-based organisms do NOT bind to receptor sites or colonize the human gut and, instead, simply pass through the digestive system in a matter of hours.
- Gut commensal spores only come alive in our gut and are fully able to bind to our receptor sites. This enables them to move slowly through our entire intestinal tract, cleaning it up from beginning to end over 3-4 weeks, before ultimately being excreted out.
If the first word on your probiotic label is Bacillus, but you're not sure if it is a gut commensal or soil-based strain, ask your retailer for help finding the right one or just get it here.
 2. Probiotics to Take with Antibiotics: Saccharomyces Boulardii
2. Probiotics to Take with Antibiotics: Saccharomyces Boulardii
(Pronounced “Sak-roe-my-sees Boo-lar-dee”.)
Fungi are also not killed by antibiotics, but, unlike gut commensal spore bacteria, it's not because they have a protective shell. It's because, by definition, antibiotics kill only bacteria.
Saccharomyces Boulardii, found in live kombucha, is a health-producing fungi. This fungal probiotic is also perfect to take with your antiobiotic as it, too, survives the pharmaceutical chemical and will continue to resist the regrowth of pathological bacteria both during and after the medication protocol.
Beyond surviving antibiotics, though, there's another big plus to taking Saccharomyces Boulardii.
It is one of the few probiotics to have been shown in clinical studies to “fight off” C. diff.
What is C. diff.? Clostridium difficile is an extremely difficult-to-treat, antibiotic-resistant, potentially lethal bacteria that “increased 400% between 2000-2007…“
Parents, did you know that taking this probiotic regularly could protect you and your family from unwanted susceptibility?!
Since C. diff. is frequently picked up at medical facilities, those at highest risk include anyone who:
- Is taking a round of antibiotics,
- Visits a doctor's office or medical clinic,
- Resides in a nursing home, and/or
- Has a stay in a hospital.
How taking antibiotics puts us at risk for getting C. Diff.
Beneficial bacteria provide protection by fighting off pathological microbes. When good bacteria get killed by the medication, it leaves us vulnerable to an invasion afterwards by “bad guys.”
That's why when it comes to which probiotics to take with antibiotics, it's so very important to take the right kinds during and after to provide extra protection during that vulnerable window post-medication.
Once the antibiotic is done, how long do you keep taking probiotics?
I would be sure to continue taking both probiotics for at least another month after finishing the medication to give beneficial bacterial residents some solid support in their regrowth period.
And personally, I take both these probiotics daily as part of an ongoing preventative approach because:
- Our immune system depends directly upon these health-promoting strains. In a perfect world, we would consume them many times a day naturally because our food would be exclusively from organic plants grown in healthy soil. Unfortunately, we have so destroyed the soil, sterilized our entire food and agricultural systems, and over-washed our food, we can no longer count on natural plant sources for these critically important gut bacteria. Our most reliable source is currently in supplement form.
 I definitely want as much protection as I can get from deadly superbugs, including C. diff. Because who knows? I may want to pop in to visit Aunt Ethel in the nursing home at a moment's notice without concern.
I definitely want as much protection as I can get from deadly superbugs, including C. diff. Because who knows? I may want to pop in to visit Aunt Ethel in the nursing home at a moment's notice without concern.
Luckily, both probiotics are 100% shelf stable so they never need refrigeration, and they travel easily too, so say goodbye to Delhi Belly and Montezuma's Revenge!
3. Which probiotics to take with antibiotics isn't the only important consideration: Also keep eating your fermented foods!
Although the vegetative bacteria strains found in fermented foods and conventional probiotics are unable to colonize in our gut, they DO, however, provide nutrition for the anaerobic bacteria (those can live without oxygen) that reside there permanently.
This is what I imagine happens in our gut when we eat fermented foods…
The anaerobic bacterial residents of our gut are hanging out on the intestinal sidelines, watching their dead aerobic cousins float by on the river of food.
“Oh, I could use that!” says one as he grabs a tool from a microbial passerby to pop into his toolbelt for use later. And all up and down the line you see this happening.
Eewww, I know, right? A bit like grave robbing!
But this IS the basic mechanism for how vegetative probiotics make us feel better. Mostly dead, but genetically similar, these bacteria provide nutritious “chemical messengers” from their biology. Microbiologists describe it more scientifically as a “genetic exchange” between the dead and live bacteria.
So, sure, belly up to that sauerkraut jar or use up that leftover bottle of conventional probiotics!
All three kinds of probiotics (gut commensal spore bacteria, probiotic fungi like Saccharomyces Boulardii, and conventional vegetative strains like lactobacillus or bifidobacterium) complement each other because each does something slightly different in the gut microbiome and so can be taken at the same time.
What else can we do to stay safe? Avoid antibiotics in our food!
Did you know that antibiotics are not only given to sick animals, but they are given to conventionally raised animals to fatten them up more quickly?! (So besides being horrible for our immune system, what else do you think that meat does to our bodies?)
Maryland has become the second U.S. state (after California) to pass a law banning the routine use of antibiotics in healthy livestock and poultry, a move aimed at battling the rise of dangerous antibiotic-resistant bacteria known as “superbugs…”
The World Health Organization has warned that human infections from antibiotic-resistant bacteria pose a grave threat to global health. Such infections are estimated to kill at least 23,000 Americans annually, although a recent Reuters investigation found that many infection-related deaths are uncounted. (Source: Maryland joins California in battling antibiotic overuse on farms)
 These are not easy issues and we have a right to make sure our families are safe from accidental exposure to these lethal strains!
These are not easy issues and we have a right to make sure our families are safe from accidental exposure to these lethal strains!
The reality is, if California and Maryland can ban the routine use of antibiotics, every state can.
We must stay focused on the real problem – overuse of antibiotics, particularly in factory farms.
Keep yourself and your family as protected as possible:
- Avoid commercially raised meat, eggs and dairy from conventional/factory farms. (If you don't have a local source for safe meat, you could order it here.)
- Eat a variety of fermented foods, and supplement with the two probiotics you've learned about today here and here.
- Test, don't guess! Insist that your doctor test first to confirm that your symptoms are caused from a bacterial infection, NOT a viral infection, before taking a round of antibiotics. (Antibiotics do nothing for viral infections.) And,
- Let your representatives know you want a ban on the routine agricultural use of antibiotics in food.
Have you ever experienced a worsening of health after a round of antibiotics?
While antibiotics absolutely have their place when facing a life-threatening situation, nevertheless I can't tell you how many stories I've heard from people who trace the onset of their current, and much more severe, symptoms back to that round of antibiotics they received for conditions like earache, chest cold or acne.
These new and different symptoms, post-antibiotic, can be almost anything:
- Digestive issues and/or new food sensitivities,
- Anxiety/depression,
- Hormonal problems,
- Autoimmune/asthma/allergies, etc.,
- Vaginal or reproductive complications,
- Skin aggravations like acne, hives, eczema, psoriasis, etc.
The key to understanding the connection is, did this new level of health challenge appear within 1-12 months after taking antibiotics?
Remember, science is not a criticism! We're all learning together, and what may have seemed like a godsend at the time, may also come with a fairly heavy price later. But thankfully we have some possible solutions in what we now know about which probiotics to take with antibiotics.
So tell us about your experiences and observations concerning antibiotic use, or perhaps what hard choices you've had to make, especially as a parent. Anything you would do differently now? If so, what? What nontoxic approaches have worked for you?
***Go here to get the probiotic that Kelly and I take.***
More you might like:
- Is My Probiotic Really Helping or am I Wasting Money? 5 Ways to Know For Sure
- One small change brought hope to this Mom's Autistic son
- Click here for posts about How We Avoid Antibiotic Bullets and More!
- Why You Should Think Twice Before Giving Your Child Antibiotics by Chris Kresser
- Can Leaky Gut be Healed? Find Out HOW: Study Showed Reversal in 30 Days
- Do Healthy Foods Make You SICK? Help for Those with Suffering with Histamine Intolerance
- 15 Ways to Keep Your Child Healthy (That your doctor never told you!)
- Suffering from eczema? I've heard this book, The Eczema Diet, is really good.
Recipes for Homemade Personal Care:
*To avoid all the antibacterial products on the market now, which even the CDC says is dangerous!
- Tons of DIY recipes in one spot
- DIY Organic Beauty Recipes E-Book
- 75 Non-toxic Recipes for Home and Beauty
Disclaimer reminder: Neither the author nor I are health professionals! Use what you read here for your own research and then maybe consult with a natural-minded doctor or health professional you trust to find what is best and right for YOU. Read my entire disclaimer here, and also note that there may be affiliate links in this post.
Photo Credits: top photo, Aunt Ethel, no antibiotics.




 I definitely want as much protection as I can get from deadly superbugs, including C. diff. Because who knows? I may want to pop in to visit Aunt Ethel in the nursing home at a moment's notice without concern.
I definitely want as much protection as I can get from deadly superbugs, including C. diff. Because who knows? I may want to pop in to visit Aunt Ethel in the nursing home at a moment's notice without concern.
Ashley says
Where do I buy this at? I looked all over on this link
KitchenKop says
Sorry, I just fixed it to hopefully make it more clear.
Go here to get the probiotics talked about in this post.
Kelly
Evelyn says
I need help.. My Mom has used abx and steroids for many different things thru the years and now realizes how bad they are…well, she has UTI, from Candida…and we are trying to treat it naturally, as she is asymptomatic…the only reason we found it, was that she is covered in a horrible rash…all over her…it tried to take over around 3 months ago…so, tht is when they gave her abx and 3 steroid shots…she is suffering miserably and we have really tried everything…I believe she is prob detoxing…she has lost 25 lbs; taking good supplements…any ideas? Thx. Evelyn
KitchenKop says
Hi Evelyn,
Sorry about all your Mom is going through.
So she is taking the probiotic in this post? Only this one has the best shot of helping her. She should work up (slowly) to take 4-5/day.
Is she open to homeopathy? That will root out these issues for the long haul, but it likely will take time.
Is she taking cod liver oil for a good anti-inflammatory? Here are the kinds I recommend: https://kellythekitchenkop.com/which-cod-liver-oil-should-you-take/
Also, here are 3 posts with more info on what to do for the rash, candida, and UTI:
https://kellythekitchenkop.com/how-to-get-rid-of-candida-naturally/
and
https://kellythekitchenkop.com/more-how-to-heal-eczema-with-homeopathy/
and
https://kellythekitchenkop.com/how-to-get-rid-of-a-uti-fast-without-drugs/
I hope all of that helps your Mom!
Kelly
Deborah says
I was wondering what the difference is if the antibiotics were given through IV. Would there be as much damage and would these two supplements be the best choice still?
KitchenKop says
Hi Deborah,
Yes, they’d be just as bad for sure, and yes, these two supplements are still what I’d take. (Remember I’m not a doctor and this isn’t medical advice, just what I’d do.)
Kelly
guest says
@ Ellen O-M Sorry hit wrong key… Like you I have also had excellent results with Just Thrive Spore Probiotic. Just Thrive is the only probiotic company that has a human clinical trial showing that – with no changes in diet or lifestyle – it reversed Leaky Gut in just 30 days at one cap daily. Furthermore, one of Just Thrive’s current ongoing clinical trials is specifically on reversing C Diff. There would be no clinical study if these gut commensal (meaning the gut is their natural home) spore bacillus strains were spreading C Diff. And yes, these strains work totally differently than streptococcus. Strep is not a spore bacillus, it is part of the lactobacillus family. The strains used in Just Thrive are extremely safe, having been being used in Europe and Asia by physicians since the 60’s as I said in the article. I’ve never heard of naturopaths saying that these strains cause a problem – only that they’ve never heard of them. Can you show me the online sources about gut commensal spore bacillus being a problem?
guest says
@ Ellen And yes, these gut commensal spore bacillus strains work very differently than strep. Similarly, they are not lactobacilli so Just Thrive is perfect for anyone with a Histamine Intolerance, SIBO or Lactobacilli overgrowth.
Ellen O'Sullivan- Mazzone says
I have tried this probiotic and it was good, however i was a little apprehensive with all of the literature regarding probiotics that are of this nature becoming opportunistic in the body and may actually spread infections etc if one was present. Also many people do not do well with a strep strain of probiotic . I was wondering if this works differently. I look forward to the feedback. Thank you
guest says
Hi Ellen! I wrote the article. Not sure what you mean about a probiotic that spreads an infection? Where did you read that? The spore bacillus used in Just Thrive have been being safely used for humans and animals since the 60’s; they have an extremely long track record of safety. “Spore” is simply a microbiological term meaning something naturally has a protective shell. It doesn’t mean it’s bad. Also, the strains used in Just Thrive are 100% “gut commensal” meaning the gut is their natural home where they come alive to do their gut cleaning work. Because our information about the gut microbiome has exploded just in the last few years, there’s still a lot of inaccurate, old information out there. For more explanation you may want to check out this article: https://kellythekitchenkop.com/is-my-probiotic-really-helping-or-wasting-money/

Ellen O'Sullivan- Mazzone says
Thank you so much for your response. There has been a lot of current research published regarding the use of spore probiotics. So much good stuff, however some naturopaths have voiced some concern on the fact that the spores can somehow spread in your gut and keep multiplying and that may not be always a positive thing when it comes to people with gut issues or c diff etc. it is too much to write but that is the simple form. I was just wondering if the gut commensal is different than regular spire probiotics. I was also wondering your input on the strep strain and how you feel that may affect people who are sensitive to

It . I look forward to hearing back. Thanks
Michelle says
Would JT be safe for pets?
guest says
Michelle, my two cats get a 1/4 cap each in their food daily. One of them had a history of fairly regular vomiting until I began giving her the Spore Probiotic in her food.
MW says
Would you recommend taking more than one of each (Just Thrive and S. Boulardi) when on an antibiotic AND and antifungal 2x per day–particularly when battling SIBO and Candida? Also, do you suggest taking BOTH at the exact same time as the antibiotic and anti-fungal? Thank you!!
guest says
@ MW Keep in mind that candida and SIBO are actually secondary symptoms. An overgrowth of either cannot occur when the numbers of the beneficial strains remains high. Just Thrive spore bacteria naturally provide nutritional support to the beneficials, thus increasing their numbers – and they do this without introducing toxic chemicals into our gut microbiome. Similarly, gut commensals spores also kill both a candida and/or lactobacilli overgrowth without the toxic effects of an antibiotic or antifungal. For more information, you might want to check out this webinar: https://wholefoodsmagazine.com/multimedia/video/free-webinar-under-microscope/
MW says
Interesting, thanks for that feedback! AND the quick response!
For the record, I am using a plant based antifungal. My functional med Dr stated that an antibiotic was, unfortunately, necessary for the SIBO. Perhaps she is wrong, However, I’m hundreds of dollars into this, so I sort of feel like I need to follow her treatment plan. :-/ I’m already swaying from it by not using the probiotic she recommends. That said, are you able to answer my questions regarding how many JT and SB to take and whether or not to take them with the antibiotic/fungal? Thanks so much!
guest says
@ MW Yes, hear ya about changing course midstream! Nevertheless, most alternative docs still don’t know about how gut commensal spores function differently from non-spore conventional probiotics… at least for now, JT is getting a ton of attention due to its recently published study showing that their finished product reversed Leaky Gut in just 30 days with no other changes in diet or lifestyle. Anyway, sorry, that technical question really needs to be addressed by a clinician. All I know is I personally wouldn’t bother with either antibiotics or antifugals until I had extensively used JT first in combination with gut microbiome testing. For more info on JT’s LG trial, see https://kellythekitchenkop.com/can-leaky-gut-be-healed-study-showed-reversal/
MW says
Thank you, SO much. I just listened to the webinar you posted above and I’m just floored! It all seems way too good to be true! I hope it’s not! 😉 I’m going to stop my antibiotic for now and see what happens with JT! Given that my antifungal is plant based, I may stick with it–I need to do a bit more research on it to decide! Thanks again!!
guest says
Rather than self-diagnosing, MW, you might want to consider contacting Dr. Tom Bayne who’s the clinician in that webinar. He’s worked with the spore strains more than anyone else in the country. I really think you need to transition carefully! Go here https://pbhealthcenter.com/about/#TomBayne
MW says
Thanks so much-I’m looking into it all very thoroughly! I am most definitely NOT self diagnosing–I’ve had oodles and oodles of tests and seen multiple drs–like I said, I’ve put hundreds of dollars into fixing this mess! I sent you an additional message via the contact me form on your website with some more specific questions.
Thanks! 🙂
Tanveer says
Hi
Your article is really helpful. There are so many new things I am learning. Much thanks for sharing these tips/ this article
Sue says
So I’m curious how you have come to this conclusion? Is this just from your own research and family experience? Please share your research sources? Thx
guest says
@ Sue I tried to provide links as much as possible. A big portion of this article is a revision of one from a couple years ago that focused on Saccharomyces Boulardii. I added new information that I’ve more recently learned about the gut commensal spores and Kelly reposted. I have been in the natural foods & products industry my entire life, plus my primary approach to healing is the natural approach, ,so my sources come from my professional life and my personal experiences pursuing my own health solutions.
Kate G. says
Can my 18 month old take this? He was an emergency C-section babe who struggles with eczema. I am concerned about his microbiome since he wasn’t inoculated through the birth canal. Any suggestions on an appropriate probiotic/spore strain will be so helpful. Thank you!
kitchenkop says
Kate I think your 18 month old can take it, just open up the capsule and sprinkle it on his food. You’ll want to start with a very little bit.
Kelly
Sandy Shallow says
My friend has sepsis. Can she take this while in ICU?
guest says
Hi Marilyn, look on Biokult’s ingredient list. One strain starts with Bacillus (subtilis) so that is a gut commensal spore; all the rest are aerobic, vegetative strains. The gut commensal spore strain used in Biokult is different than the Bacillus subtilis HU58 used in Just Thrive, though, because all the strains in JT are licensed from the top spore lab in the world, Royal Holloway. They are also all DNA-verified, tested and proprietary to Just Thrive.
Ann Toloso-Salanky says
My mother died with c-diff. It’s a horrible way to suffer & die. I wish I could’ve helped her with info like this.
guest says
@ Ann Oh Ann, I’m so very sorry for your loss! But, yes, pay it forward! You can help so many people with this information, that’s the way I look at it
:)))
Marilyn Zimmerman says
What about Biokult? Which is what I use
Debbie Thompson says
Yes, my mother-in-law had C. diff three times last year due to taking cipro for diverticulitis. Found out about the saccharomyces. She started taking that and has not had another recurrence. Wish we would have known this sooner!
guest says
@ Debbie Yikes, C Diff 3 times – your mother-in-law is lucky to have you as a researcher. Good work!